Water-based wellbeing programme also helps to improve patient flow
The benefits of water-based therapy have been well known for centuries to the Greeks, the Romans, and later the Ottomans, but you don’t have to step back in time to discover just how helpful this can be.
The rehabilitation medicine team at Castle Hill Hospital has been working with East Riding Leisure to offer access to tailored health and wellbeing programmes to aid patients’ physical mobility, balance, strength and confidence as they recovery from brain injury.
But the potential these programmes offer for other patients with ongoing health conditions or for those on elective surgery waiting lists is also huge.

Dr Yomi Salawu, consultant in rehabilitation medicine
Dr Yomi Salawu, consultant in rehabilitation medicine (pictured), tells us more:
“One of the most successful ways to help patients on their journey to recovery, or indeed to better health and wellbeing more generally, is to provide personalised care.
“Our team has been referring suitable patients to Good Boost since it launched late last year, and previously to the HealthiER exercise on prescription programme, as a means of supporting their ongoing recovery once they leave hospital.
“Good Boost comprises a range of pool and studio-based activity from leisure centres in Beverley and Driffield which can be tailored to individual needs and goals, plus there’s an option for people to take part in virtual programmes too.
“There is increasing clinical evidence of the beneficial effects of water-based activity in promoting recovery which is the hallmark of rehabilitation. The buoyancy of the water helps to support the weight of the body and reduce lower limb loading for people who need to practice walking, for example, while at the same time, the water provides resistance to help strengthen muscles.
“Other advantages of water-based activity include faster recovery and increased range of movement, and let’s not forget that hydrotherapy is also known to help with stress reduction, relaxation, and mental well-being too. It really is a holistic approach to health and recovery.”
Good Boost is available to patients with many different types of health condition or to people who would simply benefit from increased physical activity or improved mobility. As well as helping after an issue or illness has occurred, it can also be a vital tool in preparing people for elective surgery, helping patients to lose weight and lower their blood pressure, for example, to give them the best possible chance of successful surgery.
Clinicians can refer any patients they believe would benefit, at any stage of their care, or individuals can also self-refer. There is a small charge of £36.50 for access over 10 weeks, but this also includes access to virtual classes and to leisure centre facilities beyond the Good Boost organised sessions.

Good Boost can be used to aid prevention, treatment and recovery from most conditions, although not all patients will be suitable for referral; some common contraindications would include open wounds that are yet to heal (e.g. following surgery), active infections, tracheostomy, severe epilepsy, UTIs and illness such as a common cold or fever.
As well as the many benefits community-based exercise programmes like these bring for the individuals, there are also knock-on benefits for others too.
Dr Salawu continues:
“As health professionals, we know the importance of patients being fit for surgery, so use of Good Boost or similar exercise on prescription programmes can help to keep those who are waiting for an operation in good health, and help others who may not be in the best shape right now to improve the chances of their surgery being successful.
“If patients are fit, well and prepared for surgery, it reduces the number of cancellations or postponed operations, helps us maximise use of our theatres and surgical staff, and helps maintain timely access to surgery for other patients.
“From the perspective of my team working in rehabilitation, the delivery of programmes like these has really helped to reduce pressure on the community rehabilitation team and enabled them to see those with the most pressing needs more quickly.

“We started to see this during the COVID pandemic when leisure centres supported the physical aspects of Long Covid rehab and recovery programmes. Over time, this type of programme has continued and been extended out to more patients and conditions beyond just Long Covid, and we have continued to see benefits in both our team capacity and our patient services.
“As waiting lists for Good Boost are short, suitable patients can now access physical activity sessions earlier than they could be seen by the community therapists, which is better for them, but it also allows the community therapists to focus on the higher risk and more disabled patients for whom the leisure centre sessions would not be suitable.
“What’s also really important is that this type of programme gives people the chance to have a say in and take responsibility for their own health. Many of our patients leaving hospital are keen to continue their recovery and regain their independence, they want structure and they’re highly motivated, so this type of programme can be really empowering for those who just want to keep going without having to wait for community services either.”
Good Boost is suitable for a wide range of people, from those who are pregnant or post-partum through to people with back pain, arthritis, those on elective waiting lists and those looking to improve mobility and coordination.
An informal drop-in session for both referrers and potential participants will be held this coming Monday 7th April at 1pm at Beverley Leisure Centre. More details about the programme will be available, plus there will be the opportunity for hands-on demonstrations of the tablets used by participants, and suitable referrals can be taken on the day.
If you’re unable to attend, you can find out more from the Good Boost website or from Caroline Duke, Healthy Lifestyle Development Officer /call 07800 783593.










 A hospital screening service is appealing to people in East Yorkshire and Northern Lincolnshire to overcome their embarrassment so they can be checked for bowel cancer.
A hospital screening service is appealing to people in East Yorkshire and Northern Lincolnshire to overcome their embarrassment so they can be checked for bowel cancer. The faecal immunochemical test (FIT) examines a sample of your poo for blood, one of the signs of bowel cancer.
The faecal immunochemical test (FIT) examines a sample of your poo for blood, one of the signs of bowel cancer. 



 A specialist in infectious diseases in Hull is warning cases of Tuberculosis (TB) are increasing, with homeless people or those with drug or alcohol addictions at risk.
A specialist in infectious diseases in Hull is warning cases of Tuberculosis (TB) are increasing, with homeless people or those with drug or alcohol addictions at risk.
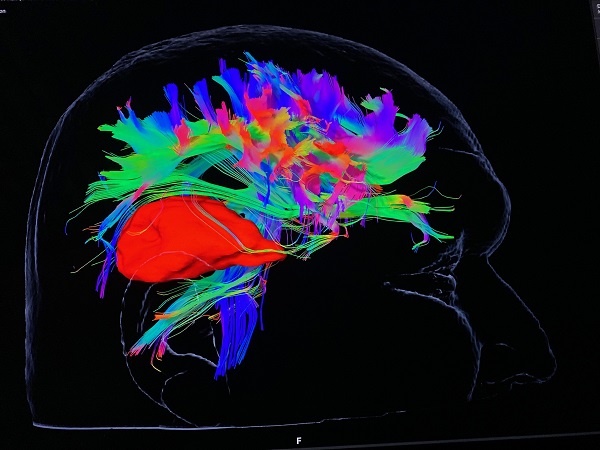
 Consultant Neurosurgeon Chittoor Rajaraman said: “For the first time in Hull, we will be able to use this technology to offer patients safer surgery, with better outcomes.
Consultant Neurosurgeon Chittoor Rajaraman said: “For the first time in Hull, we will be able to use this technology to offer patients safer surgery, with better outcomes.



